The question of when to start breast cancer screening for average risk individuals has been a hot topic in recent years in Canada, so I wanted to take some time to present the current recommendations and their rationale. I will also be providing information about the topic of breast cancer in general and about breast cancer screening.
Screening Recommendations
United States
In the United States, the U.S. Preventative Services Task Force changed their recommendations in 2024 to recommend that women between 40 and 74 years old receive screening every 2 years. This was changed from its previous guidelines that advised starting at 50 years old.
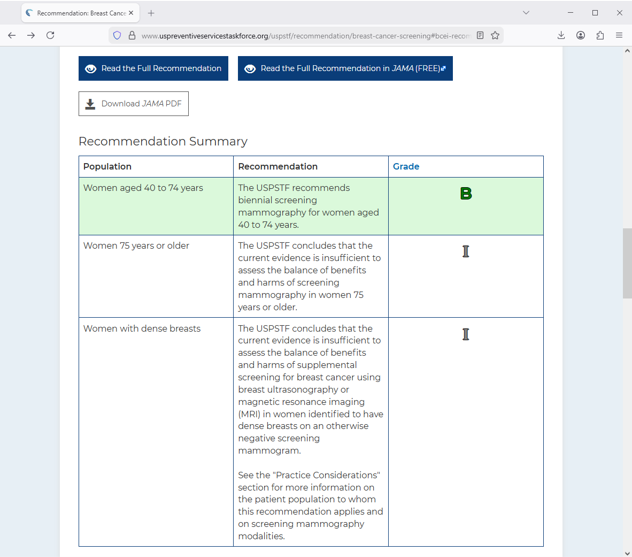
Source
The reason for this change in the guidelines is due to the rise in breast cancer in the under 50 age group in the US.
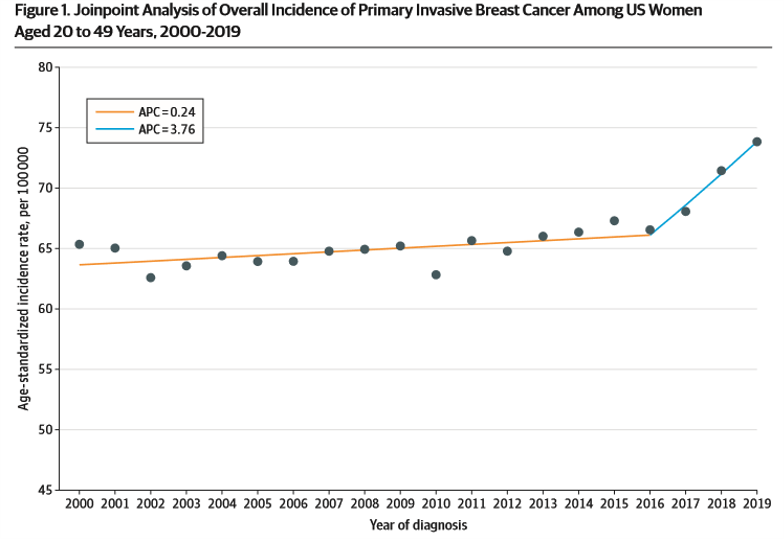
Source: https://jamanetwork.com/journals/jamanetworkopen/fullarticle/2814306
Canada
This worrying increasing trend of breast cancer unfortunately has also been observed in Canada.
These graphs show the in the under 50 age group from 1984 to 2019.
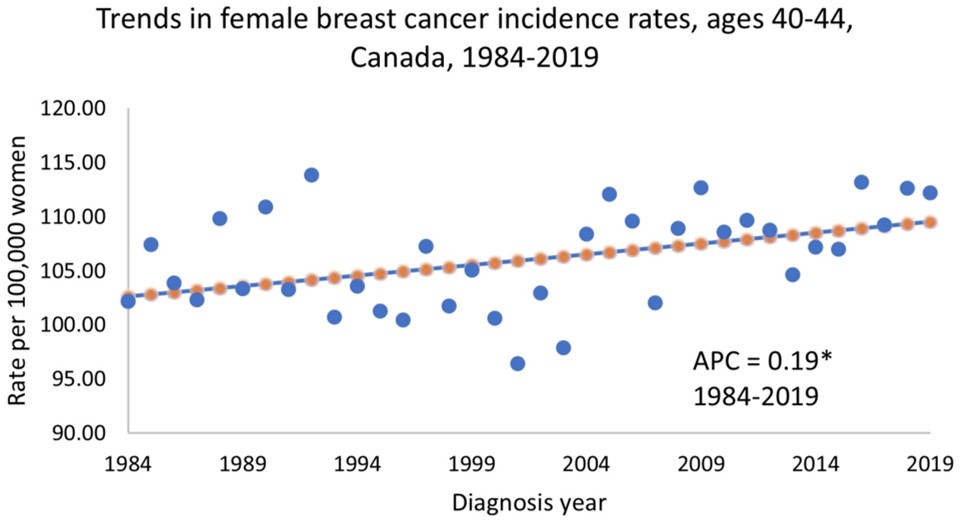
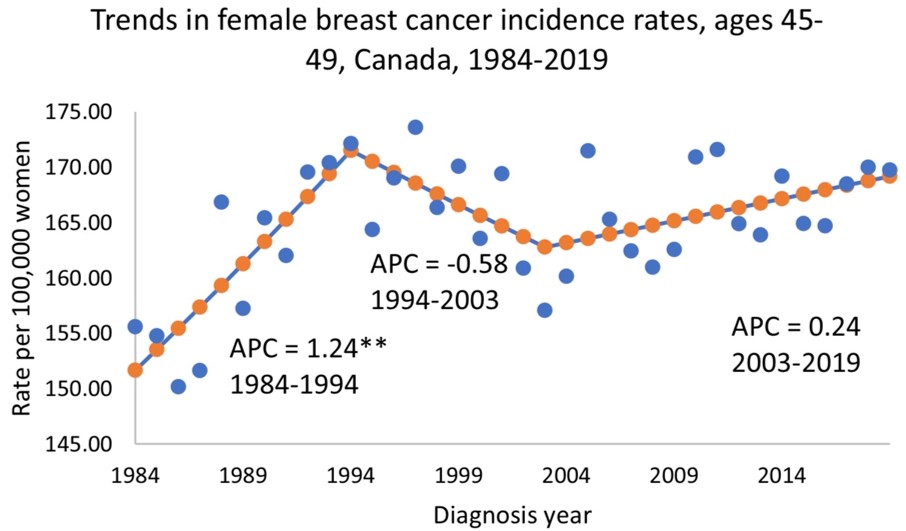
Source: https://journals.sagepub.com/doi/10.1177/08465371241246422
In Canada, the Canadian Cancer Society has adopted the same recommendations of the US Preventative Services Task force that women between the ages of 40 and 74 get screened every two years.
Source: https://cancer.ca/en/cancer-information/find-cancer-early/get-screened-for-breast-cancer/when-should-i-be-screened-for-breast-cancer
The Canadian Task Force on Preventive Health Care’s draft guidelines differ slightly in that they suggest screening every 2-3 years for women aged 50 to 74. For women aged 40-49, they suggest against systemically screening, but those who choose to be screened after being informed of the benefits and harms should be offered screening every 2 to 3 years.
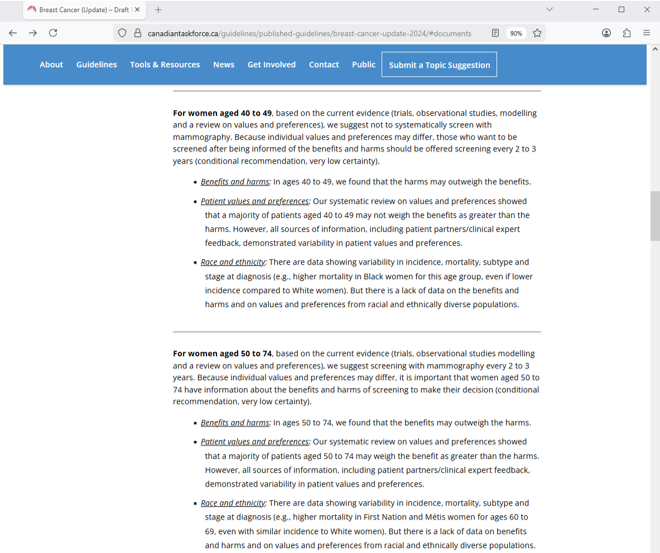
Source: https://canadiantaskforce.ca/guidelines/published-guidelines/breast-cancer-update-2024
The difference in how they worded their recommendations stems from the fact that Canadian statistics show that breast cancer risk increases as women age, making the benefits of screening clearer for those between 50 and 74. For women in their 40s, the decision is more nuanced, so the Task Force emphasizes personal choice rather than a blanket recommendation.
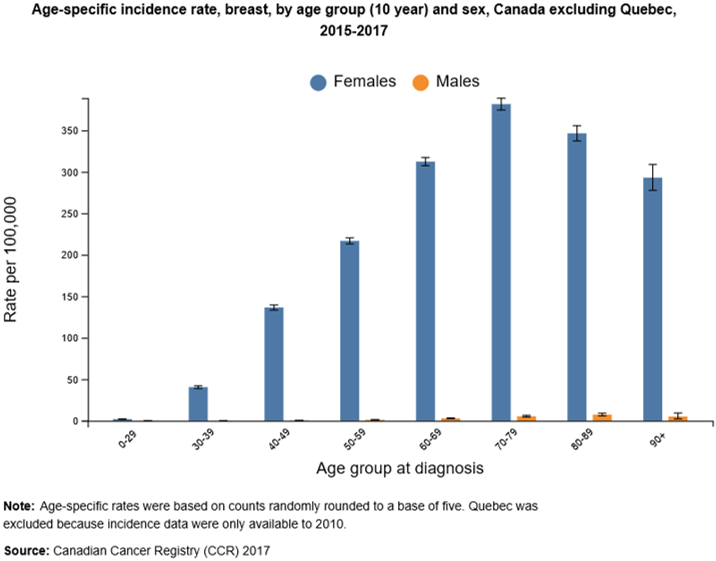
Canadian Breast Cancer Screening Programs
In Canada, Provincial and Territorial Screening Programs organize screening tests for breast cancer.
Depending on the region, 2 programs may be available, one for people with an average risk of developing breast cancer and one for higher risk individuals.

Risk Factors for Breast Cancer
People who may fall into the high-risk category:
- People with a personal or extensive family history of breast cancer. Here family is referring to blood-related family members. People with a personal or family history of ovarian cancer is also at higher risk.
- Individuals with a high risk gene mutation or has a family member with this mutation are also at higher risk.
- Individuals who have received radiation therapy to the chest to treat another cancer such as Hodgkin’s Lymphoma before the age of 30 and more than 8 years ago are at higher risk as well.
If you have any of these above four risk factors, your primary care provider will be able to provide you with further information regarding high-risk screening options. This could mean starting screening even earlier than 40 years old and screening on a yearly basis.
Other factors that may increase someone’s risk of developing breast cancer:
- Certain characteristics of the breast such as having dense breasts also increases the risk of breast cancer.
- If you were previously diagnosed with a benign breast disease, your risk of breast cancer is also higher.
- Starting periods younger than 12 years old and starting menopause at more than 55 years old can also increase risk of breast cancer. This is because the exposure to the fluctuating hormones of estrogen and progesterone during each menstrual cycle can increase the risk of cancerous changes in the breast. So the more menstrual cycles you have had in your life, the higher your risk of breast cancer.
- Not having children increases the long-term risk of breast cancer. The risk of breast cancer is also increased in women who have children later in life, such as 35 years or older.
Modifiable risk factors that may increase someone’s risk of developing breast cancer:
Most of what I have listed so far are factors that are difficult to control. Here are the factors that can be changed, things that you can do to reduce your chance of getting breast cancer:
- Alcohol consumption and tobacco use increase the risk of many different types of cancers, and this includes breast cancer.
- Exposures to certain chemicals such as BPA and phthalates, among others can also increase risk of breast cancer.
- Menopausal hormone therapy if used for more than 5 years can increase breast cancer risk.
- Lifestyle factors such as having a BMI of over 30 and having a sedentary lifestyle and having irregular sleeping habits can also increase the risk.
This is not an exhaustive list of risk factors and there may be other things that increase breast cancer risk that are not listed here.
Risk Estimate Calculators for Breast Cancer
If you are interested in a personalized risk estimate calculator for breast cancer, there are 2 links that you can use to find out:
The second link can incorporate your breast density in the calculator, which improves the accuracy of the estimate if you have this information.
Provincial and Territorial Screening Programs
I am going to discuss mostly about the Average Risk Breast Cancer Screening programs offered by most regional screening programs in Canada.
As you can see here, each province or territory’s screening program has its own recommendations for when to start screening and how frequently to test, and this does ultimately determine an individual’s overall ease of access to breast cancer screening.
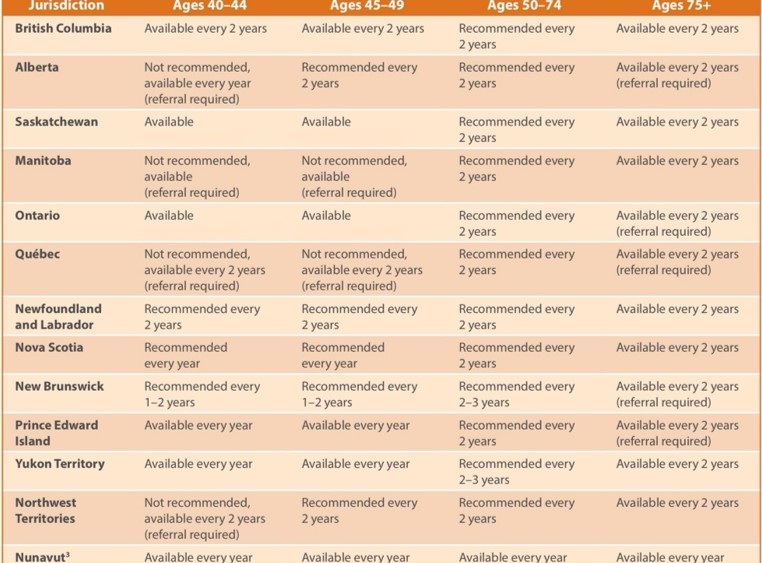
Source: https://canadianprimarycaretoday.com/article/view/2-3-Arthur_et_al
The exact eligibility criteria for each region’s screening program differs slightly from one another, but one thing they all share in common is that people with breast cancer symptoms are not eligible. This is because screening is a test for people with no symptoms of the disease that they are being tested for. People who have symptoms, would have to go to their primary care provider to get a diagnostic test, not a screening test.
Breast Cancer Symptoms
So what are breast cancer symptoms that would prompt a visit to the doctor?
- Lump
The most obvious symptom would be a tangible lump in the breast or in the armpit since there are lymph nodes here that can get enlarged when breast cancer is present - New nipple inversion or Skin Dimple
When the underlying cancer attaches to the overlying skin, it can pull the skin towards it inwards which can cause a dimple.
If this occurs near the nipple, it can cause the nipple to retract inwards - Abnormal nipple discharge
The surface of the nipple has multiple exit openings for the milk ducts. If any of these openings leak abnormal fluid spontaneously such as blood, it can be a sign of cancer. - Skin changes (redness, sores or crusting, or thickening)
A certain type of breast cancer called Inflammatory breast cancer can cause skin redness, sores or crusting.
Another type of skin change from breast cancer can be skin thickening, with the skin appearing like the surface of an orange, due to swelling caused by the cancer blocking the lymphatic drainage system. - One-sided breast size changes such as one side becoming bigger or smaller or changing in shape, can also occur with breast cancer
- Breast pain
Breast cancer may not always present with all of these symptoms. Any of these symptoms could indicate breast cancer.
Breast Cancer Screening Eligibility
Breast cancer screening is available to:
- 40-74 y.o. (depending on the province)
- Who were born female or is transfeminine with at least 5 consecutive years of hormone use
Frequency of Breast Cancer Screening
- 1-2 years (depending on the province)
Depending on the province, the frequency of testing ranges between every 1 to 2 years for people are average risk.
However people with high density breasts may be advised to undergo screening after 1 year even if they are in a region that generally recommend biennial screening.
You may find out after your first mammogram how dense your breasts are when you receive your results.
Breast Density
This picture shows the differences in densities of breasts of 4 different people.
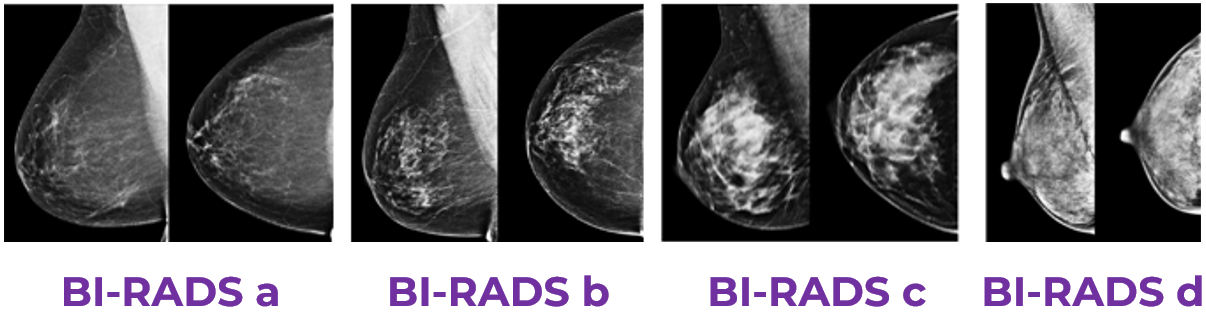
Source: ACR BI-RADS® Atlas, 5th edition, pp. 128-130
A is low density and D is the highest density category.
Breast cancer usually appears white on the mammogram, so in higher density breasts which have more white areas overall, it would be harder to see an abnormal lump. So people with dense breasts may get diagnosed with breast cancer later when it has grown bigger.
Generally people who are younger tend to have higher density breasts. Around half of women over 40 years old have dense breasts.
People of Asian descent also tend to have denser breasts.
Notably, having dense breasts is a risk factor for breast cancer.
Screening Mammogram
The imaging test used is called a screening mammogram which involves an X-ray of the breast. The person getting screened has their breast placed one at a time between 2 plates which squeeze together to flatten the breast for 10 to 15 seconds. The pictures need to be taken from two different angles so this squeezing will occur twice for each breast, from top to bottom and from side to side.
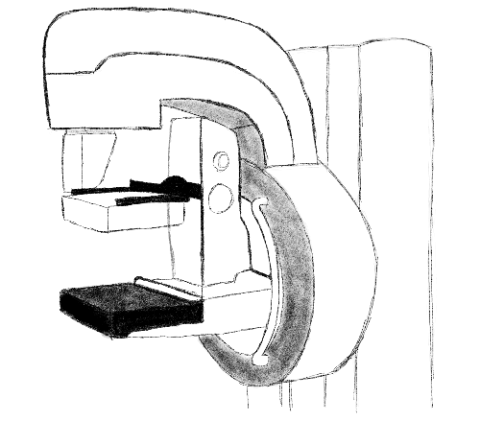
Benefits of Breast Cancer Screening
Getting screened regularly can help find breast cancer before a lump can be felt by hand.
This image shows the average size of breast cancer lumps by the method of detection. It shows here that the average size of a lump found through regular mammogram screening is 1.1 cm, however the mammogram has the ability to detect even smaller masses that cannot be felt at all. This image is not to scale.
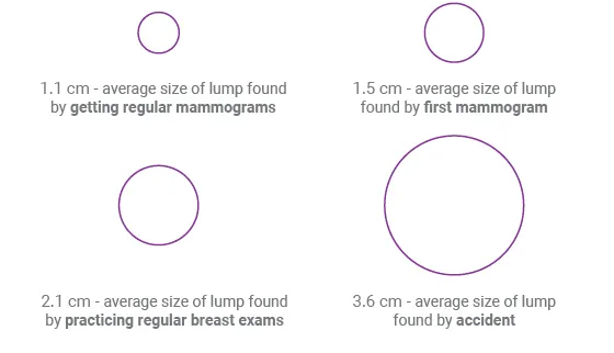
Source: https://www.mammotome.com/us/en/patient-resources/understanding-mammograms
This degree of early detection means that the cancer has less time to spread. So it could lead to:
- A lower chance of dying from breast cancer
Detecting cancer through a screening mammogram does not guarantee that the cancer will be cured, but it may help with the odds of survival.
This graph shows the 5-year survival rate in percentages with the stages of when the cancer was diagnosed. We can clearly see that the survival rates are better when the cancer is detected in the early stages with the highest 5-year survival rate at stage 1 in blue which is close to 100 percent.
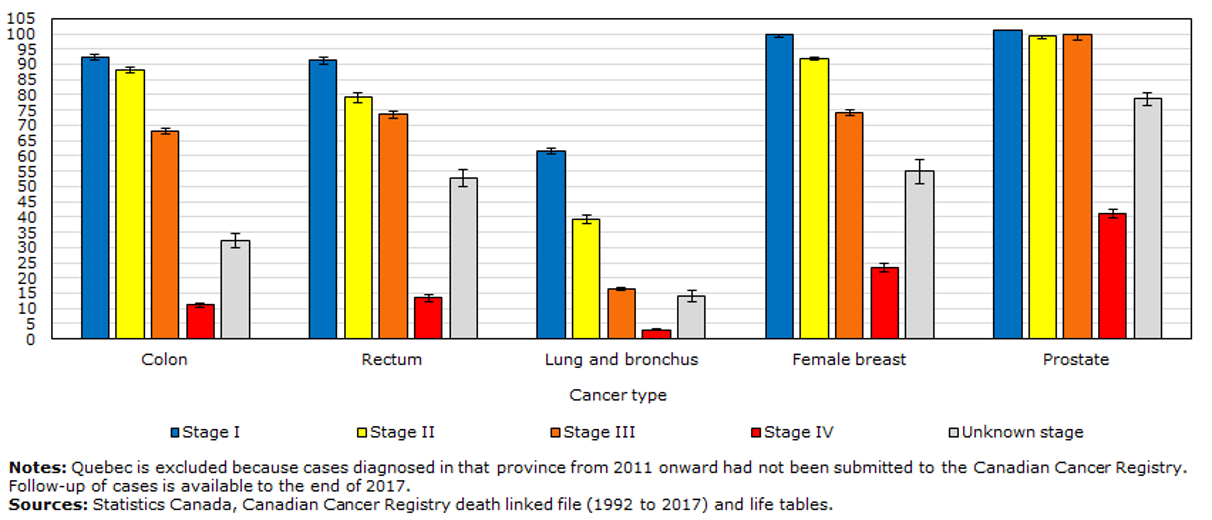
- Better outcome with treatment
- Fewer and less invasive treatments
Potential Harms of Breast Cancer Screening
False Positive result leading to additional tests
Sometimes a healthy individual undergoing a screening mammogram can get an abnormal mammogram result even though they do not have breast cancer. This is called a false positive result.
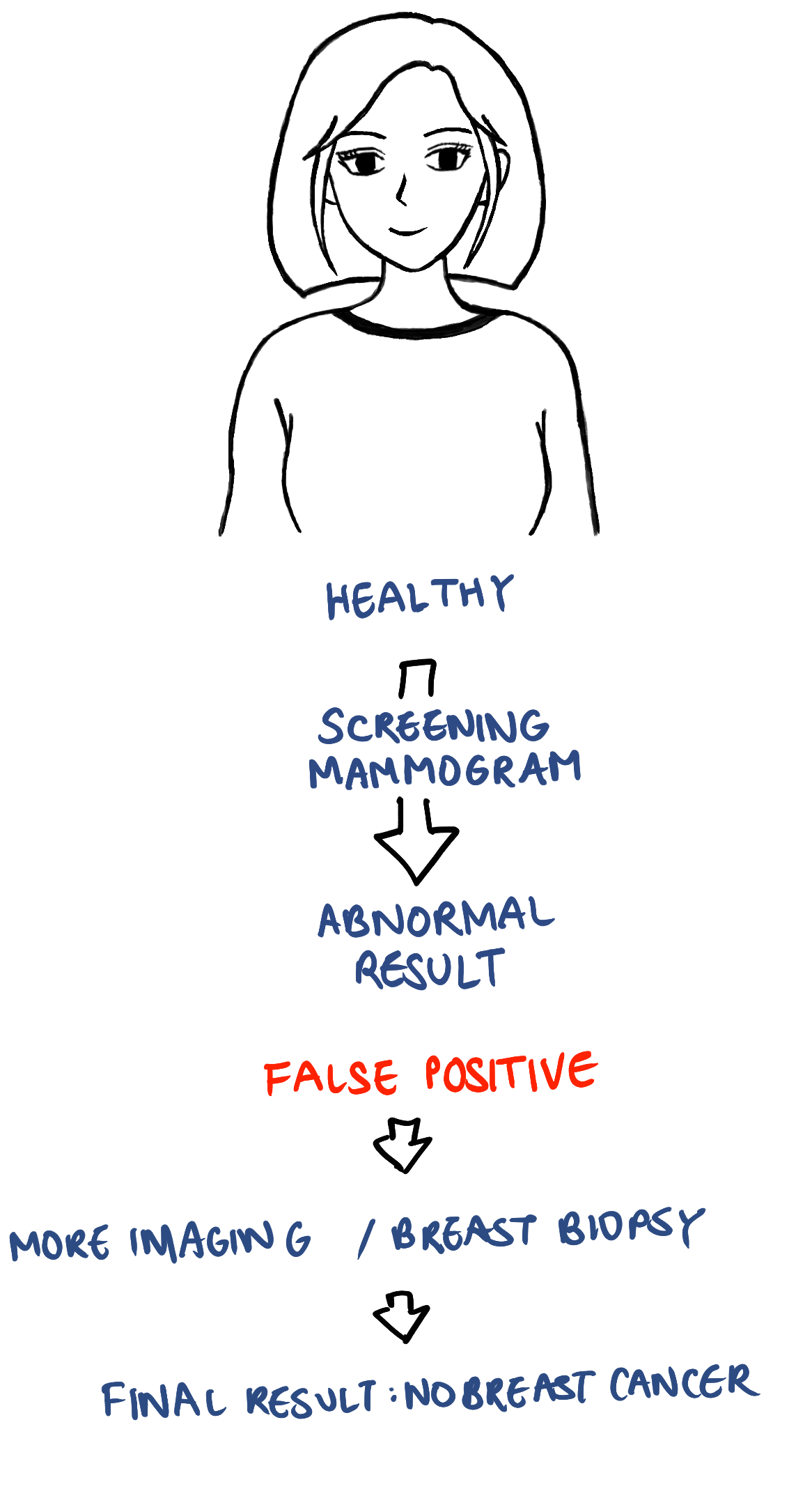
False positive results can lead to additional imaging tests or a biopsy, with the final result of these tests showing that there is no breast cancer.
In most cases, the only additional test required would be a diagnostic mammogram which takes additional views of a specific area of interest. Sometimes the additional test required is a breast ultrasound or a breast MRI.
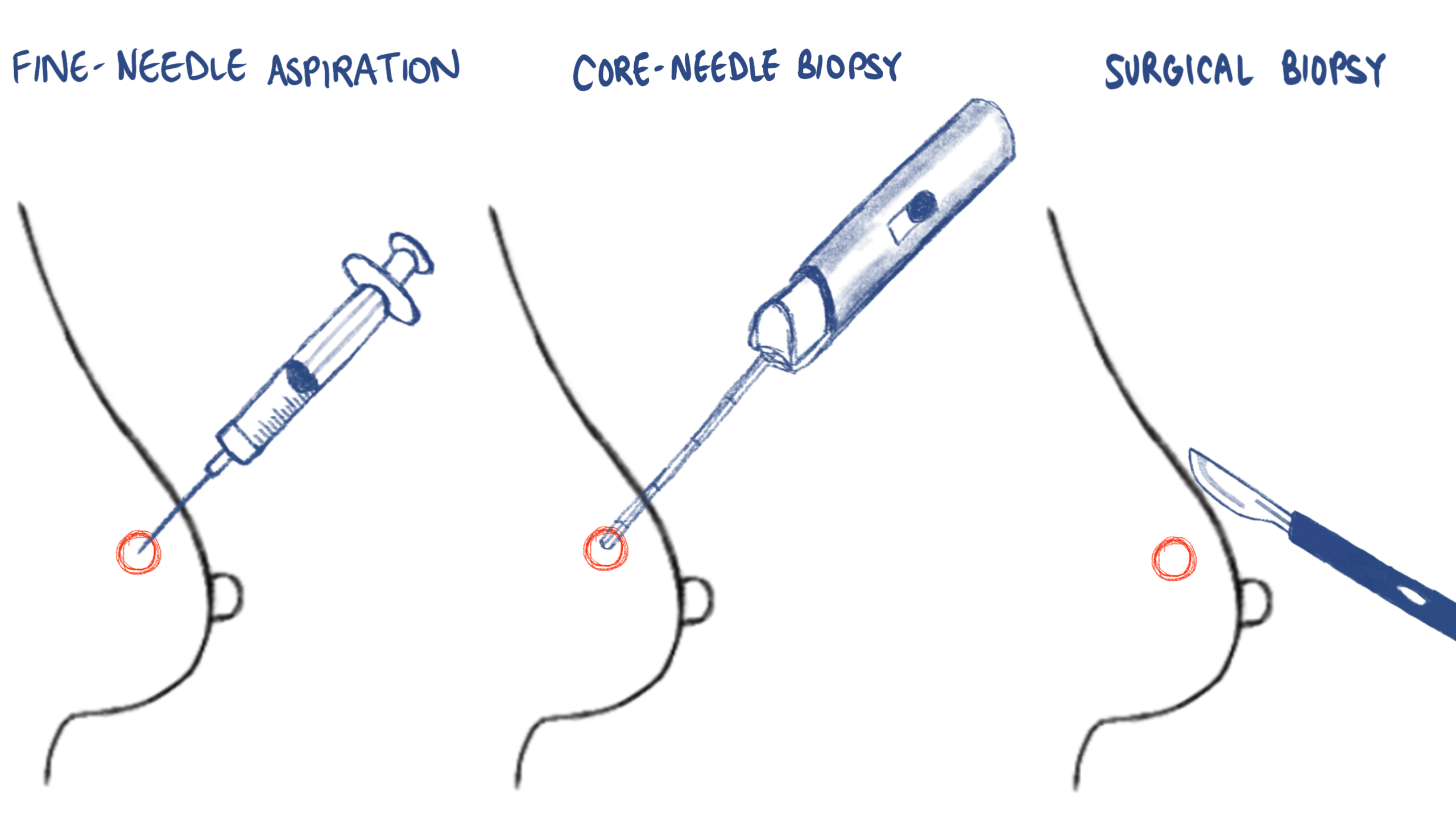
When a breast biopsy is needed, a sample of the abnormal area is taken out to check for cancer. There are different ways of getting this sample, but most commonly it is taken out through a small procedure called a Core-Needle Biopsy that uses a hollow needle under local anesthesia.
False positive results occur more commonly if:
- It is the first mammogram and there are no previous mammograms for comparison. Being called for these additional tests may be anxiety-provoking for some, but one thing to note is that if someone was called back for additional views after the first mammogram, it is less likely to happen again on the next mammogram since there is a previous mammogram to compare it to.
- Taking estrogen
- Younger age
- High breast density
- Breast biopsies in the past
- Family history of breast cancer
False negative result leading to a false sense of security
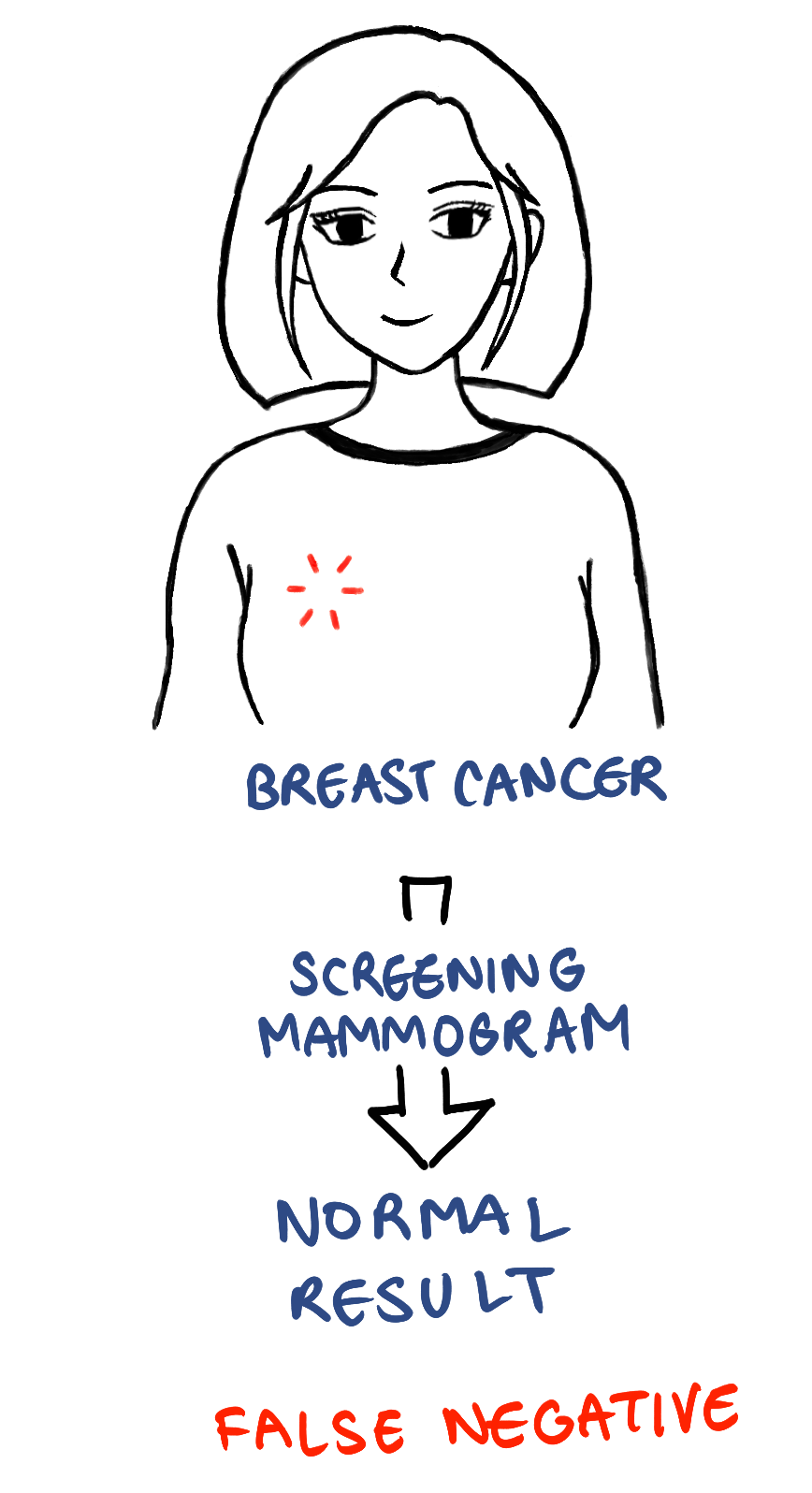
Screening mammograms can sometimes miss breast cancer, which can lead to someone getting a normal result even though breast cancer is present. This can cause a false sense of security in the person being tested and cause them to believe that they are healthy when they in fact have breast cancer. So if you have symptoms, it is important to go to your primary care provider even if you had a normal mammogram recently so that they can then order more specific tests for your symptoms.
Over-diagnosis
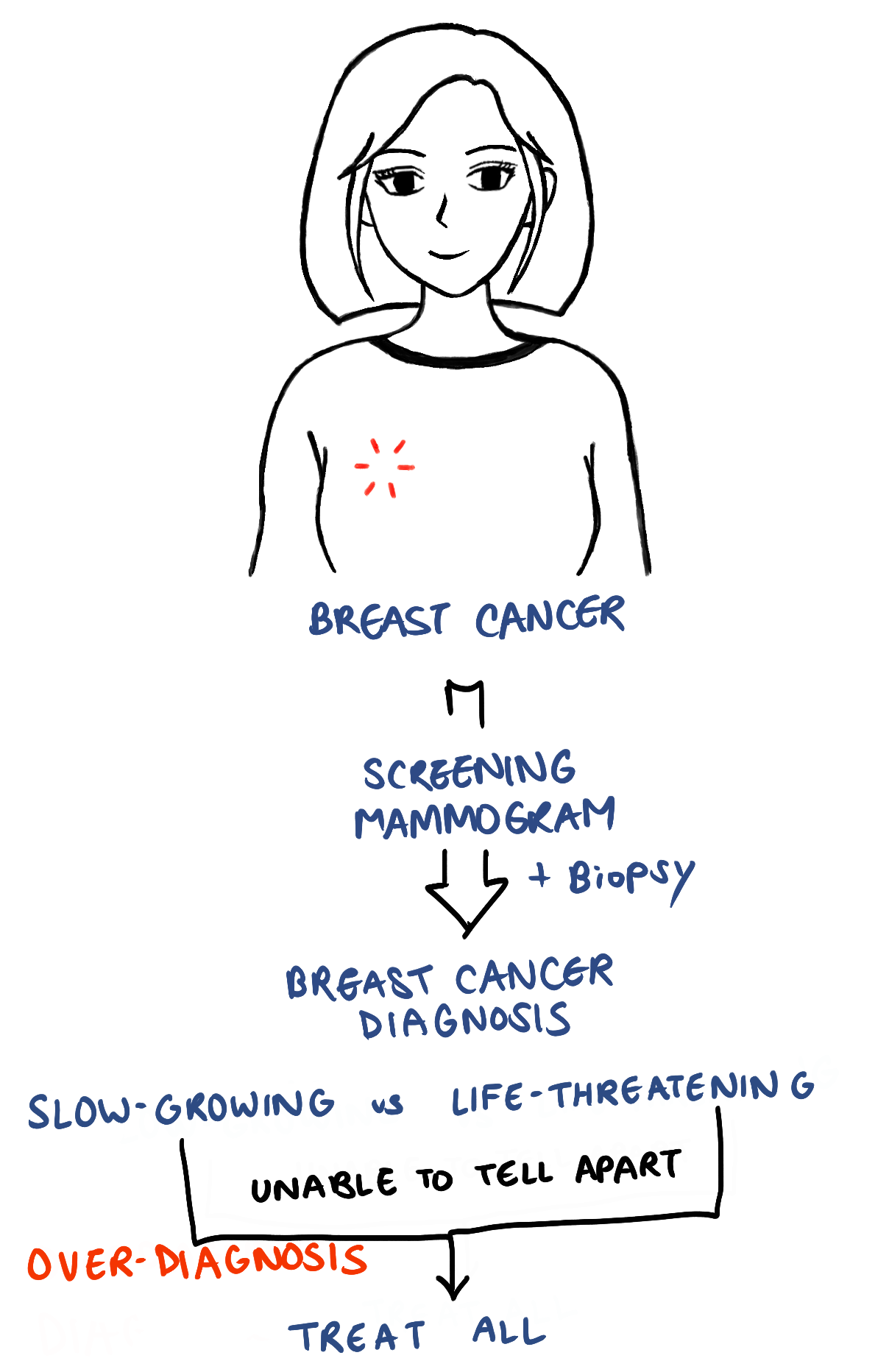
Over-diagnosis is when a screening mammogram finds breast cancer that would have grown too slowly to spread and the patient would not have died from it if left untreated. However these cancers cannot be distinguished from those that do cause death, so doctors would not risk not treating it. In these circumstances, these patients may be exposed to the negative side effects of cancer treatment that may not have been needed in the first place.
This also brings up the important topic of discussing with the doctor the question about continuing breast cancer screening if the individual considering screening is already suffering from a life threatening health problem. Detecting breast cancer early may not necessarily increase the life expectancy or improve their quality of life if they are already very sick. In these individuals, it may be that they would pass away with breast cancer, and not from it, limiting the test’s usefulness.
Radiation exposure
Mammograms use X-rays so it exposes the breasts to a low dose of radiation. People are often concerned about radiation exposure due to fears that it will increase the long-term risk of cancer.
However, to get a better idea of the degree of radiation exposure someone is exposed to with one screening 2D mammogram, it is helpful to have some context.
Canadians are exposed to an average of about 1.8 mSv per year from natural surroundings. Some example sources of this background radiation is cosmic radiation, terrestrial radiation and radon exposure. There’s even tiny amounts of radiation in the foods we eat.
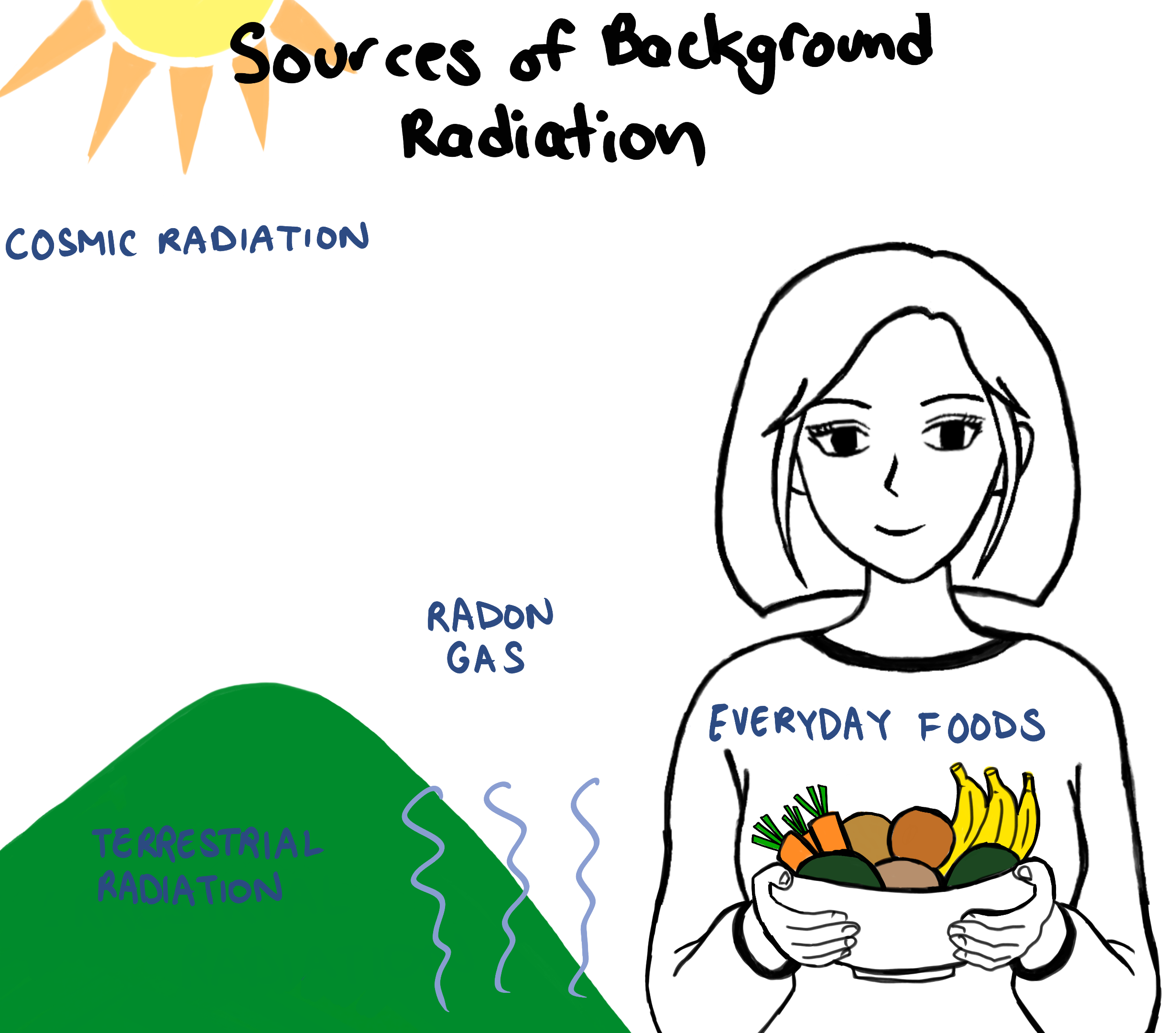
The total dose for a typical screening 2D mammogram with 2 views of each breast is about 0.4 mSv.
This means that the dose of radiation from a screening mammogram is about the same as one would get from natural surroundings in Canada over about 12 weeks.
Another way to look at it is, a 10-hour flight has similar radiation exposure to 1 chest X-ray and a mammogram is around the same amount as 4 chest X-rays. So it’s like taking a 10 hour flight 4 times.
Benefits and Risks can differ depending on the age screening is started…
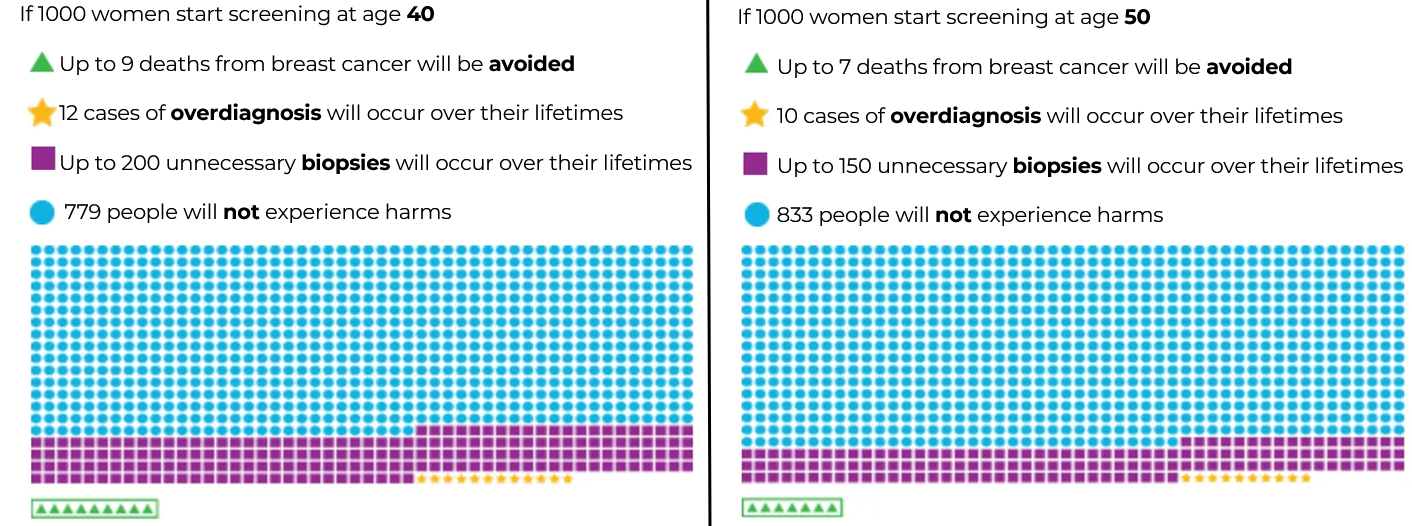
Now that you know about the benefits and risks of getting a screening mammogram, you might be curious to know how many lives are saved from breast cancer through screening or how often these cases of over-diagnosis or false positives occur. This chart gives us an estimate based on modelling using US data to predict the approximate numbers.
As you can see in this info-graphic, the benefits and risks can be different depending on when you start screening.
Source: https://www.cancercareontario.ca/en/types-of-cancer/breast-cancer/screening/ages-40-49-what-you-need-to-know
If we take for instance 2 groups of 1,000 women, and one group starts screening regularly at age 40 and the other group starts at age 50.
- Up to 9 lives from that group of 1000 will be saved from breast cancer if screening is started at 40 years old, which is 2 more lives saved in every 1000 women screened compared to the group starting at 50 years old.
- Over-diagnosis may occur in 12 women for the group starting at 40, while there are 10 in the group starting at 50 years old.
- There would be up to 200 unnecessary biopsies in the group starting at 40 year old, which is 50 more compared to the group starting at 50 years old. It is important to remember that these numbers are not referring to the results of a screening mammogram done once at 40 years old. It is estimating the total number of biopsies if these individuals started screening at 40 and continued to get screened up to 75 years of age. In other words, for the group of 1000 women starting screening at 40 years old, if we were to follow them over 35 years of screening, there would up to 200 unnecessary biopsies in this group of 1000 women in these 35 years whereas for the other group starting at 50 years old, there would be 150 unnecessary biopsies in 25 years.
- The great majority of the people in both groups will not experience any harms from breast cancer screening, indicated by the blue circles.
Personalized Assistance
If you would like personalized assistance that incorporates your values and preferences to help you decide whether to undergo screening now or to defer screening, please see your primary care provider.
If at the end, you decide not to start screening now, you can always change your mind at anytime.
If you have already made the decision to get screened, click on the link to your region’s breast cancer screening program at the bottom of the page to find out more about how to book your mammogram.
Tips to Prepare for a Mammogram
For people who have an upcoming mammogram appointment, here are some tips to prepare for the test.
- Try to go to the same imaging centre as before if you had a mammogram in the past. This will reduce your chance of getting a false positive as the radiologist will have access to the previously taken mammogram pictures for comparison. If you are unable to return to the same centre, try to bring the images or have the imaging sent from the previous imaging centre to your current one.
- If possible, try to schedule your test for when your breasts aren’t likely to be tender or swollen. The week before the menstrual period is usually the most uncomfortable for most people.
- On the day of the exam, don’t apply deodorant, antiperspirant, powders, or creams on your armpits, or on your breasts because they can show up on the images as white spots.
- Wear a 2 piece outfit like a skirt or pants, so that you’ll only need to remove your top and bra for the test
- Let the technologist know if:
- you have breast implants or have a history of a breast surgery
- you are pregnant or breastfeeding
- Avoid a screening mammogram 3 months after giving birth as there are changes in the breast tissue which can result in it being less effective. However, anyone experiencing any breast cancer symptoms after delivery can go to their primary care provider for diagnostic tests.
Helpful Resources/References
These resources were a great source of information, and I hope that it will be helpful to you too.
General Information
- Dense Breasts Canada
- American Cancer Society Breast Cancer Information
- Atlas of breast cancer early detection by the WHO: For real pictures of breast cancer, click here.
- Breast Cancer Risk Calculators
Information Regarding Impact of Race/Ethnicity on Breast Cancer
- Breast cancer incidence and mortality, by age, stage and molecular subtypes, by race/ethnicity in Canada
- Race, Ethnicity and Indigeneity in Breast Cancer | Cancer Care Ontario
Breast Cancer Screening Programs by Province/Territory
- Alberta
- British Columbia
- Manitoba
- New Brunswick
- Newfoundland and Labrador
- Northwest Territories
- Nova Scotia
- Nunavut: See your local family doctor/nurse practitioner
- Ontario: Click on Wait Times to select your mammogram centre with the shortest wait time
- Prince Edward Island
- Quebec
- Saskatchewan
- Yukon