Benefits and Risks
Benefits of Breast Cancer Screening
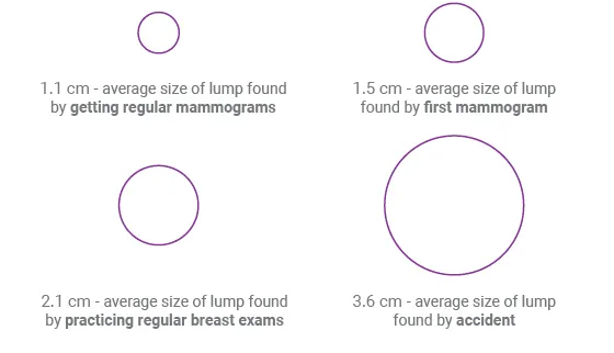
Getting screened regularly can help find breast cancer before a lump can be felt by hand.
This image shows the average size of lumps by the method of detection. It shows here that the average size of a lump found through regular mammogram screening is 1.1 cm, however the mammogram has the ability to detect even smaller masses that cannot be felt at all. This image is not to scale.
This degree of early detection means that the cancer has less time to spread. So it could lead to:
A lower chance of dying from breast cancer
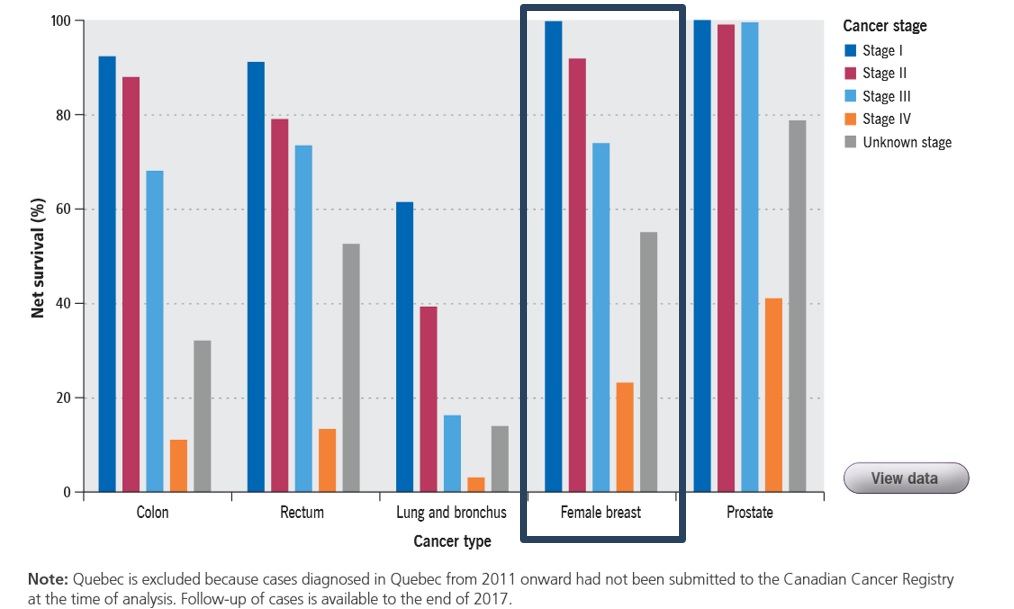
Detecting cancer through a screening mammogram does not guarantee that the cancer will be cured, but it may help with the odds of survival.
This graph shows the 5-year survival rate in percentages with the stages of when the cancer was diagnosed. We can clearly see that the survival rates are better when the cancer is detected in the early stages with the highest 5-year survival rate at stage 1 in blue which is close to 100 percent.
Better outcome with treatment
Fewer and less invasive treatments
In a medical context, the term invasive refers to anything that enters the body in a physical way, usually by breaking the skin or entering through a natural opening.
A less invasive treatment could mean making a smaller cut during surgery or limiting the area involved, thereby lowering the risk and shortening the recovery time.
In the context of breast cancer treatment, an example of a less invasive treatment is a lumpectomy, which removes only the specific area of the breast containing the lump, rather than a mastectomy, which removes the entire breast.

Finding breast cancer early can make less‑invasive treatment options possible.
Potential Harms of Breast Cancer Screening
False Positive result leading to additional tests
Sometimes a healthy individual undergoing a screening mammogram can get an abnormal mammogram result even though they do not have breast cancer. This is called a false positive result.
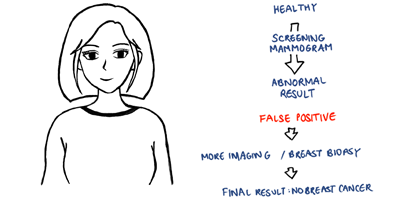
False positive results can lead to additional imaging tests or a biopsy, with the final result of these tests showing that there is no breast cancer.
In most cases, the only additional test required would be a diagnostic mammogram which takes additional views of a specific area of interest. Sometimes the additional test required is a breast ultrasound or a breast MRI.
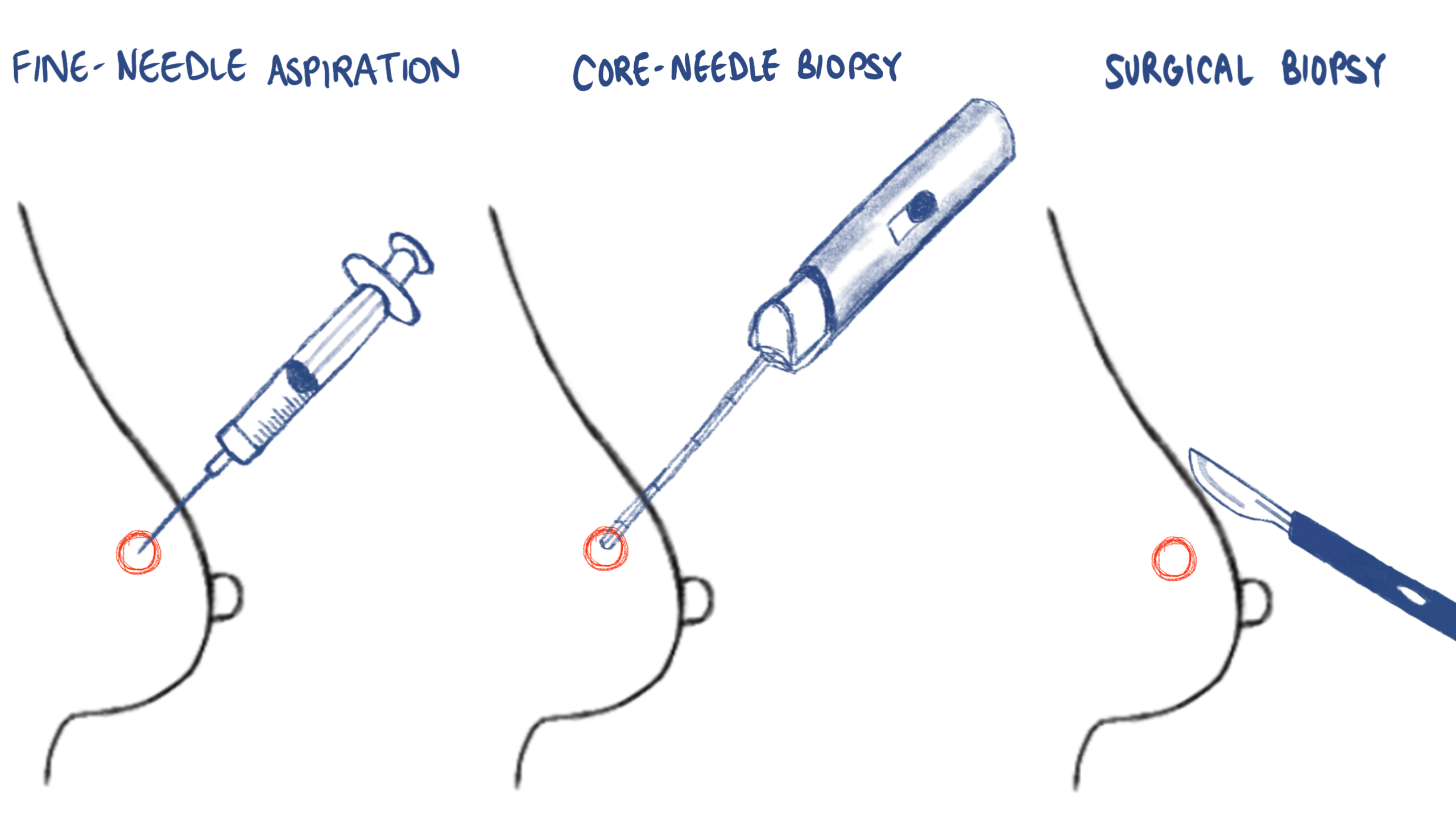
When a breast biopsy is needed, a sample of the abnormal area is taken out to check for cancer. There are different ways of getting this sample, but most commonly it is taken out through a small procedure called a Core-Needle Biopsy that uses a hollow needle under local anesthesia.
False positive results occur more commonly if:
- It is the first mammogram and there are no previous mammograms for comparison. Being called for these additional tests may be anxiety-provoking for some, but one thing to note is that if someone was called back for additional views after the first mammogram, it is less likely to happen again on the next mammogram since there is a previous mammogram to compare it to.
- Taking estrogen
- Younger age
- High breast density
- Breast biopsies in the past
- Family history of breast cancer
False negative result leading to a false sense of security
Screening mammograms can sometimes miss breast cancer, which can lead to someone getting a normal result even though breast cancer is present. This can cause a false sense of security in the person being tested and cause them to believe that they are healthy when they in fact have breast cancer. So if you have symptoms, it is important to go to your primary care provider even if you had a normal mammogram recently so that they can then order more specific tests for your symptoms.
Over-diagnosis
Over-diagnosis is when a screening mammogram finds breast cancer that would have grown too slowly to spread and the patient would not have died from it if left untreated. However these cancers cannot be distinguished from those that do cause death, so doctors would not risk not treating it. In these circumstances, these patients may be exposed to the negative side effects of cancer treatment that may not have been needed in the first place.
This also brings up the important topic of discussing with the doctor the question about continuing breast cancer screening if the individual considering screening is already suffering from a life threatening health problem. Detecting breast cancer early may not necessarily increase the life expectancy or improve their quality of life if they are already very sick. In these individuals, it may be that they would pass away with breast cancer, and not from it, limiting the test’s usefulness.
Radiation exposure
Mammograms use X-rays so it exposes the breasts to a low dose of radiation. People are often concerned about radiation exposure due to fears that it will increase the long-term risk of cancer.
However, to get a better idea of the degree of radiation exposure someone is exposed to with one screening 2D mammogram, it is helpful to have some context.
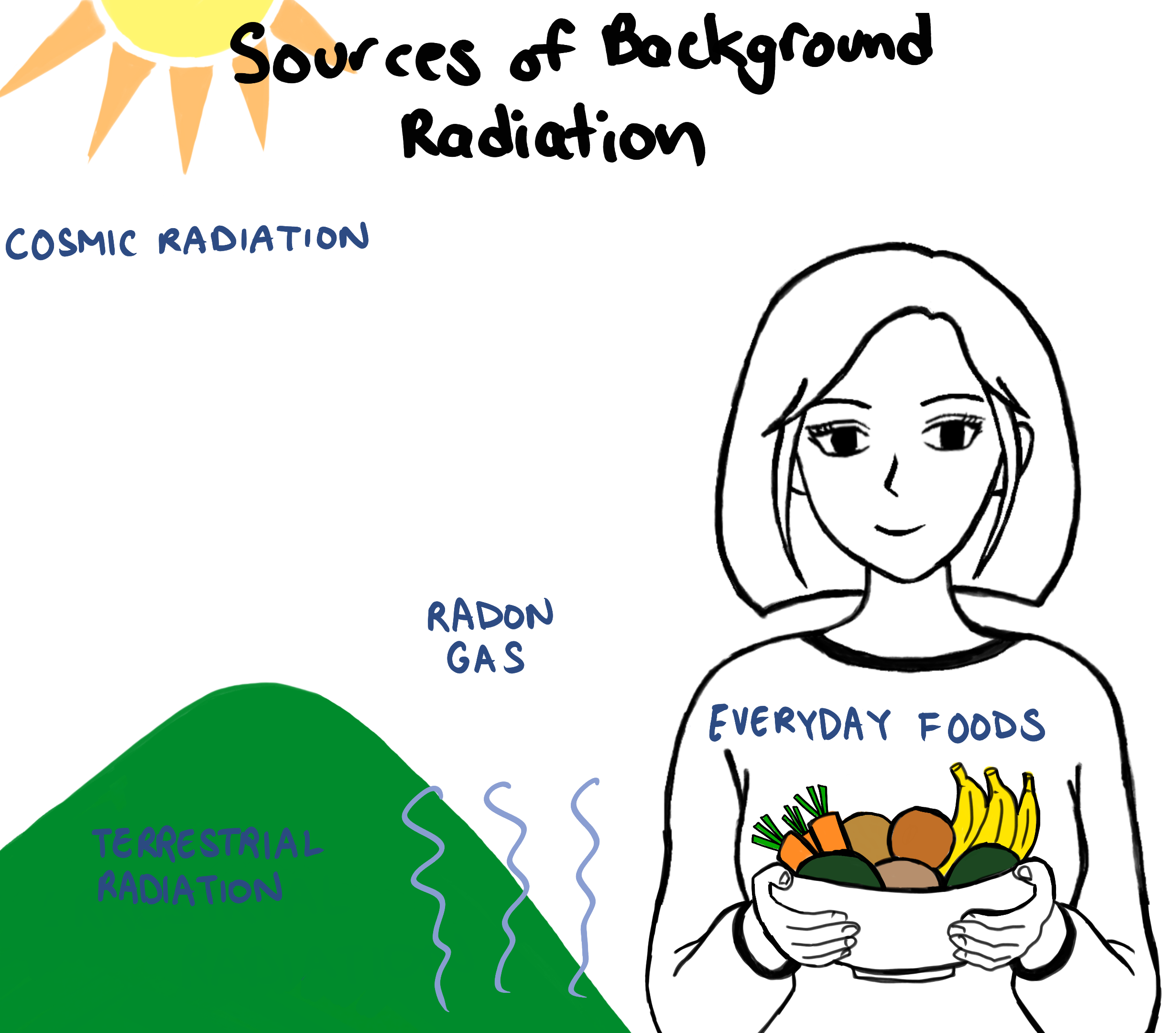
Canadians are exposed to an average of about 1.8 mSv per year from natural surroundings. Some example sources of this background radiation is cosmic radiation, terrestrial radiation and radon exposure. There’s even tiny amounts of radiation in the foods we eat.
The total dose for a typical screening 2D mammogram with 2 views of each breast is about 0.4 mSv.
This means that the dose of radiation from a screening mammogram is about the same as one would get from natural surroundings in Canada over about 12 weeks.
Another way to look at it is, a 10-hour flight has similar radiation exposure to 1 chest X-ray and a mammogram is around the same amount as 4 chest X-rays. So it’s like taking a 10 hour flight 4 times.
Benefits and Risks can differ depending on the age screening is started…
Now that you know about the benefits and risks of getting a screening mammogram, you might be curious to know how many lives are saved from breast cancer through screening or how often these cases of over-diagnosis or false positives occur. This chart gives us an estimate based on modelling using US data to predict the approximate numbers.
As you can see in this info-graphic, the benefits and risks can be different depending on when you start screening.
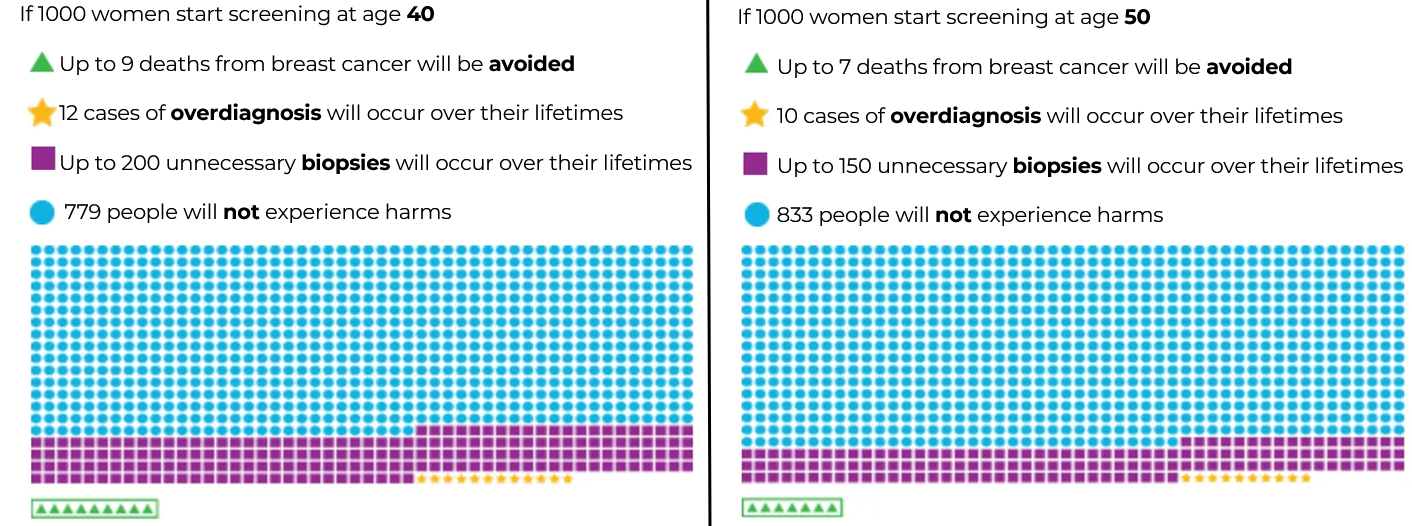
If we take for instance 2 groups of 1,000 women, and one group starts screening regularly at age 40 and the other group starts at age 50.
- Up to 9 lives from that group of 1000 will be saved from breast cancer if screening is started at 40 years old, which is 2 more lives saved in every 1000 women screened compared to the group starting at 50 years old.
- Over-diagnosis may occur in 12 women for the group starting at 40, while there are 10 in the group starting at 50 years old.
- There would be up to 200 unnecessary biopsies in the group starting at 40 year old, which is 50 more compared to the group starting at 50 years old. It is important to remember that these numbers are not referring to the results of a screening mammogram done once at 40 years old. It is estimating the total number of biopsies if these individuals started screening at 40 and continued to get screened up to 75 years of age. In other words, for the group of 1000 women starting screening at 40 years old, if we were to follow them over 35 years of screening, there would up to 200 unnecessary biopsies in this group of 1000 women in these 35 years whereas for the other group starting at 50 years old, there would be 150 unnecessary biopsies in 25 years.
- The great majority of the people in both groups will not experience any harms from breast cancer screening, indicated by the blue circles.
Personalized Assistance
If you would like personalized assistance that incorporates your values and preferences to help you decide whether to undergo screening now or to defer screening, please see your primary care provider.
If at the end, you decide not to start screening now, you can always change your mind at anytime.
If you have already made the decision to get screened, click on the link below to your region’s breast cancer screening program to find out more about how to book your mammogram.
For people who have an upcoming mammogram appointment, refer to the Tips for Preparing for a Mammogram.
Breast Cancer Screening Programs by Province/Territory
- Alberta
- British Columbia
- Manitoba
- New Brunswick
- Newfoundland and Labrador
- Northwest Territories
- Nova Scotia
- Nunavut: See your local family doctor/nurse practitioner
- Ontario: Click on Wait Times to select your mammogram centre with the shortest wait time
- Prince Edward Island
- Quebec
- Saskatchewan
- Yukon